My name is Eoghan Gubbins-Cloney. My journey with cancer began on 3rd October 1997 when, at just sixteen months old, I was diagnosed with Medulloblastoma; a brain tumour associated with the Cerebellum (base of brain).
My symptoms were not indicative of a brain tumour, my GP initially misdiagnosed me as having Cerebral Palsy, a condition which would account for the loss of control in my lower limbs but not projectile vomiting which I was also experiencing. My mom and grandmother, not completely satisfied with the Cerebral Palsy diagnosis, brought me to Cork University Hospital for a specialist second opinion. I was administered a CT scan which initially showed nothing out of the ordinary. Following this, I was given contrast before another CT scan was performed. Contrast is a dye used in CT scans to assist radiologists in distinguishing different structures in the body. With the aid of contrast, the radiologists and doctors were able to identify a golf ball-sized tumour attached to my brain stem under the Cerebellum and two metastases that had travelled to the spine.
The outlook was not good.
The doctors recommended that I should be taken home,
made as comfortable as possible and enjoy whatever time I had left;
they estimated a maximum of three weeks.
A surgeon at Cork University Hospital agreed to carry out an excision and remove the tumour, however there was no guarantee I would survive the surgery. Surgery such as this was not normally carried out on anyone under the age of two and my surgeon had never before operated on anyone as young as sixteen months for this brain tumour. However, thankfully, the surgery was a success. What followed was a course of Chemotherapy, both intravenous (3 months) and oral (5 months, administered every day by my mom). Between the IV and Oral Chemotherapy sessions, I was given 30 sessions of radiation therapy on my head and spine to eradicate metastases which had detached from the main tumour and traveled down the spinal cord. I was also placed on a new experimental protocol in Europe, whereby instead of receiving a transfusion of blood from a donor after IV chemotherapy, I received my own blood which had been taken before my chemotherapy was administered. This removed the risk of my body rejecting the blood transfusion and the adverse effects associated with that outcome.
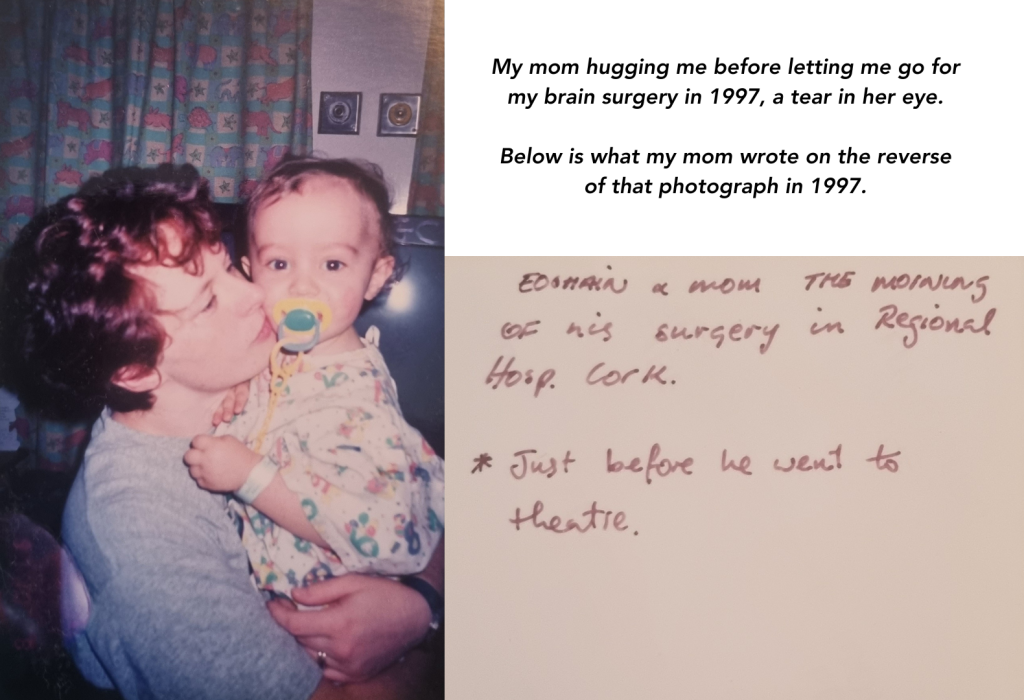

Following the successful excision and cancer treatment, I spent the next number of years travelling with my mom and family to Our Lady’s Childrens Hospital in Crumlin, Dublin for annual check-ups. I appeared to be meeting important milestones in my development and so apart from the odd mole removal, the years after my brain surgery were relatively uneventful. Then, during a growth spurt in my early teens, I was seen to have developed Kyphosis, an exaggerated curvature of the spine. All spines have that ‘S’ shape, but mine was more pronounced than is normally expected. As I grew the curvature became worse and I would eventually be seen to have developed Scoliosis in my lower back. While surgery was considered the last option, I was scheduled to go for spine surgery in 2013 to correct the curve and prevent it from getting worse as other preventative measures I had tried, such as wearing a back brace 24/7, did not work. Two titanium rods were grafted to my spine in 2013 and replaced in 2016 after an incident left the first set of rods compromised.
In 2019, I was diagnosed with a rare skin cancer; Fibroepithelioma of Pinkus. Coincidentally, right before I started my M.Sc in Cancer Research in University of Galway. Go figure. Following additional mole removals, a dermatologist familiar with my medical history suggested that we research a condition called Gorlin’s Syndrome. This is a rare genetic condition which can increase a person’s risk of developing skin cancer. I had my blood taken for the purpose of gene testing, without going for gene counselling (which as we discovered later is the incorrect order to do these things in; the gene counselling comes before the gene testing). Nevertheless, as well as conclusively having a defect in my genes indicative of Gorlin’s Syndrome (SUFU gene; a tumour suppressor gene (coincidentally, defects in this gene have been linked to the development of Medulloblastoma)) as shown in the genetic results, I also had three symptoms associated with Gorlin’s Syndrome; history of Scoliosis, the development of basal cell carcinomas (Fibroepithelioma of Pinkus) and the development of Medulloblastoma. This is what had initially led my mom’s dermatologist to suggest that I may have Gorlin’s syndrome; he was aware I had Medulloblastoma as a child under the age of two and that I had developed a rare skin cancer not typical of someone my age.
While somewhat in shock, this genetic diagnosis has brought with it a weird sense of closure; after almost two decades of asking myself why I developed brain cancer at such a young age, I finally had an answer. Going forward, I am more determined than ever to take preventative measures to limit my chances of developing skin cancer: I am wearing moisturizer with SPF on my face and exposed areas of my skin whenever I leave the house and I am staying as covered up as possible when outdoors. This coupled with increased self-monitoring and mole mapping means that I have a much greater chance of identifying cancer early if it should ever develop again.


I am able to tell my story due to the persistence of my mom, but also because of research into cancer and cancer treatment methods. I hope to use my knowledge and experience gained from my year-long M.Sc in Cancer Research in any way I can to further efforts in the pursuit of effective treatments for cancer.
It is an honour to be able to advocate for vital cancer research and support cancer charities like Breakthrough Cancer Research by raising funds to assist them in developing new ways of diagnosing and treating different cancer types, specifically those with poorer prognoses. I hope that my story has informed and inspired others. My success story for cancer research is nearly 27 years old, I cannot fathom how far research has come since then and I am so excited to see where it goes in the coming years and decades.









 Contact
Contact